The Circulatory System: A Closed Network of Blood Vessels and the Heart


The circulatory system is an essential part of the human body that ensures that all the organs and tissues receive the oxygen and nutrients they need to function
- Uploaded on | 3 Views
-
 alexishughes
alexishughes
About The Circulatory System: A Closed Network of Blood Vessels and the Heart
PowerPoint presentation about 'The Circulatory System: A Closed Network of Blood Vessels and the Heart'. This presentation describes the topic on The circulatory system is an essential part of the human body that ensures that all the organs and tissues receive the oxygen and nutrients they need to function. The key topics included in this slideshow are . Download this presentation absolutely free.
Presentation Transcript
Slide1The Circulatory SystemThe Heart, Blood Vessels, Blood Types
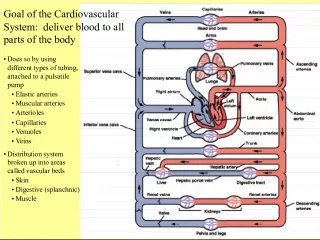
Slide2The Closed Circulatory System• Humans have a closed circulatory system , typical of all vertebrates, in which blood is confined to vessels and is distinct from the interstitial fluid. – The heart pumps blood into large vessels that branch into smaller ones leading into the organs. – Materials are exchanged by diffusion between the blood and the interstitial fluid bathing the cells.
Slide3The Cardiovascular System• Three Major Elements – Heart, Blood Vessels, & Blood – 1. The Heart - cardiac muscle tissue – highly interconnected cells – four chambers • Right atrium • Right ventricle • Left atrium • Left ventricle
Slide5Pathway of the blood• Superior Vena Cava • Right Atrium • Tricuspid Valve • Right Ventricle • Pulmonary Semilunar Valve • Lungs • Pulmonary Vein • Bicuspid Valve • Left Ventricle • Aortic Semilunar Valve • Aorta • To the bodies organs & cells
Slide6Circuits• Pulmonary circuit – The blood pathway between the right side of the heart, to the lungs, and back to the left side of the heart. • Systemic circuit – The pathway between the left and right sides of the heart.
Slide7The Cardiovascular System2. Blood Vessels -A network of tubes – Arteries arterioles move away from the heart • Elastic Fibers • Circular Smooth Muscle – Capillaries – where gas exchange takes place. • One cell thick • Serves the Respiratory System – Veins Venules moves towards the heart • Skeletal Muscles contract to force blood back from legs • One way values • When they break - varicose veins form
Slide9The Cardiovascular System3. The Blood A. Plasma Liquid portion of the blood. Contains clotting factors, hormones, antibodies, dissolved gases, nutrients and waste
Slide10The Cardiovascular System• The Blood B. Erythrocytes - Red Blood Cells – Carry hemoglobin and oxygen. Do not have a nucleus and live only about 120 days. – Can not repair themselves.
Slide11The Cardiovascular System• The Blood C. Leukocytes – White Blood cells – Fight infection and are formed in the bone marrow – Five types – neutrophils, lymphocytes, eosinophils, basophils, and monocytes.
Slide12The Cardiovascular SystemThe Blood • D. Thrombocytes – Platelets. – These are cell fragment that are formed in the bone marrow from magakaryocytes . – Clot Blood by sticking together – via protein fibers called fibrin.
Slide13Disorders of the Circulatory System• Anemia - lack of iron in the blood, low RBC count • Leukemia - white blood cells proliferate wildly, causing anemia • Hemophilia - bleeder’s disease, due to lack of fibrinogen in thrombocytes • Heart Murmur - abnormal heart beat, caused by valve problems • Heart attack - blood vessels around the heart become blocked with plaque, also called myocardial infarction
Slide14Unit 9 – The HeartCardiovascular System The Heart The Heart
Slide15Functions of the Heart• Generating blood pressure • Routing blood – Heart separates pulmonary and systemic circulations • Ensuring one-way blood flow – Heart valves ensure one-way flow • Regulating blood supply – Changes in contraction rate and force match blood delivery to changing metabolic needs
Slide16Size, Shape, Locationof the Heart • Size of a closed fist • Shape – Apex : Blunt rounded point of cone – Base : Flat part at opposite of end of cone • Located in thoracic cavity in mediastinum
Slide17Heart Cross Section
Slide18Pericardium
Slide19Heart Wall• Three layers of tissue – Epicardium : This serous membrane of smooth outer surface of heart – Myocardium : Middle layer composed of cardiac muscle cell and responsibility for heart contracting – Endocardium : Smooth inner surface of heart chambers
Slide20Heart Wall
Slide21External Anatomy• Four chambers – 2 atria – 2 ventricles • Auricles • Major veins – Superior vena cava – Pulmonary veins • Major arteries – Aorta – Pulmonary trunk
Slide22External Anatomy
Slide23Coronary Circulation
Slide24Heart Valves• Atrioventricular – Tricuspid – Bicuspid or mitral • Semilunar – Aortic – Pulmonary • Prevent blood from flowing back
Slide25Heart Valves
Slide26Function of the Heart Valves
Slide27Blood Flow Through Heart
Slide28Systemic and PulmonaryCirculation
Slide29Heart Skeleton• Consists of plate of fibrous connective tissue between atria and ventricles • Fibrous rings around valves to support • Serves as electrical insulation between atria and ventricles • Provides site for muscle attachment
Slide30Cardiac Muscle• Elongated, branching cells containing 1-2 centrally located nuclei • Contains actin and myosin myofilaments • Intercalated disks : Specialized cell-cell contacts • Desmosomes hold cells together and gap junctions allow action potentials • Electrically, cardiac muscle behaves as single unit
Slide31Conducting System of Heart
Slide32Electrical Properties• Resting membrane potential ( RMP ) present • Action potentials – Rapid depolarization followed by rapid, partial early repolarization. Prolonged period of slow repolarization which is plateau phase and a rapid final repolarization phase – Voltage-gated channels
Slide33Action Potentials inSkeletal and Cardiac Muscle
Slide34SA Node Action Potential
Slide35Refractory Period• Absolute : Cardiac muscle cell completely insensitive to further stimulation • Relative : Cell exhibits reduced sensitivity to additional stimulation • Long refractory period prevents tetanic contractions
Slide36Electrocardiogram• Action potentials through myocardium during cardiac cycle produces electric currents than can be measured • Pattern – P wave • Atria depolarization – QRS complex • Ventricle depolarization • Atria repolarization – T wave: • Ventricle repolarization
Slide37Cardiac Arrhythmias• Tachycardia : Heart rate in excess of 100bpm • Bradycardia : Heart rate less than 60 bpm • Sinus arrhythmia : Heart rate varies 5% during respiratory cycle and up to 30% during deep respiration • Premature atrial contractions : Occasional shortened intervals between one contraction and succeeding, frequently occurs in healthy people
Slide38Alterations in Electrocardiogram
Slide39Cardiac Cycle• Heart is two pumps that work together, right and left half • Repetitive contraction ( systole ) and relaxation ( diastole ) of heart chambers • Blood moves through circulatory system from areas of higher to lower pressure. – Contraction of heart produces the pressure
Slide40Cardiac Cycle
Slide41Events during Cardiac Cycle
Slide42Heart Sounds• First heart sound or “lubb” – Atrioventricular valves and surrounding fluid vibrations as valves close at beginning of ventricular systole • Second heart sound or “dupp” – Results from closure of aortic and pulmonary semilunar valves at beginning of ventricular diastole, lasts longer • Third heart sound (occasional) – Caused by turbulent blood flow into ventricles and detected near end of first one-third of diastole
Slide43Location of Heart Valves
Slide44Mean Arterial Pressure (MAP)• Average blood pressure in aorta • MAP=CO x PR – CO is amount of blood pumped by heart per minute • CO=SV x HR – SV : Stroke volume of blood pumped during each heart beat – HR : Heart rate or number of times heart beats per minute • Cardiac reserve: Difference between CO at rest and maximum CO – PR is total resistance against which blood must be pumped
Slide45Factors Affecting MAP
Slide46Regulation of the Heart• Intrinsic regulation : Results from normal functional characteristics, not on neural or hormonal regulation – Starling’s law of the heart • Extrinsic regulation : Involves neural and hormonal control – Parasympathetic stimulation • Supplied by vagus nerve, decreases heart rate, acetylcholine secreted – Sympathetic stimulation • Supplied by cardiac nerves, increases heart rate and force of contraction, epinephrine and norepinephrine released
Slide47Heart Homeostasis• Effect of blood pressure – Baroreceptors monitor blood pressure • Effect of pH, carbon dioxide, oxygen – Chemoreceptors monitor • Effect of extracellular ion concentration – Increase or decrease in extracellular K + decreases heart rate • Effect of body temperature – Heart rate increases when body temperature increases, heart rate decreases when body temperature decreases
Slide48Baroreceptor and ChemoreceptorReflexes
Slide49Baroreceptor Reflex
Slide50Chemoreceptor Reflex-pH
Slide51Effects of Aging on the Heart• Gradual changes in heart function, minor under resting condition, more significant during exercise • Hypertrophy of left ventricle • Maximum heart rate decreases • Increased tendency for valves to function abnormally and arrhythmias to occur • Increased oxygen consumption required to pump same amount of blood